Diabetic Foot: Why a Vascular Surgeon is Your Feet’s Best Friend
If you have diabetes, you’ve likely been told to check your feet every day. But if a complication arises—like a wound that won’t heal, a change in skin color, or a persistent ache—you might wonder who the right specialist is. While podiatrists and wound care experts are vital, the Vascular Surgeon plays a unique and critical role in saving the diabetic foot.
Here is why a vascular specialist is the “anchor” of your foot health team.
It’s All About the "Fuel Lines"
- Angioplasty and Stenting: Using tiny balloons to widen narrowed arteries from the inside.
- Bypass Surgery: Creating a new path for blood to flow around a blockage.
Preventing the "Silent" Threat
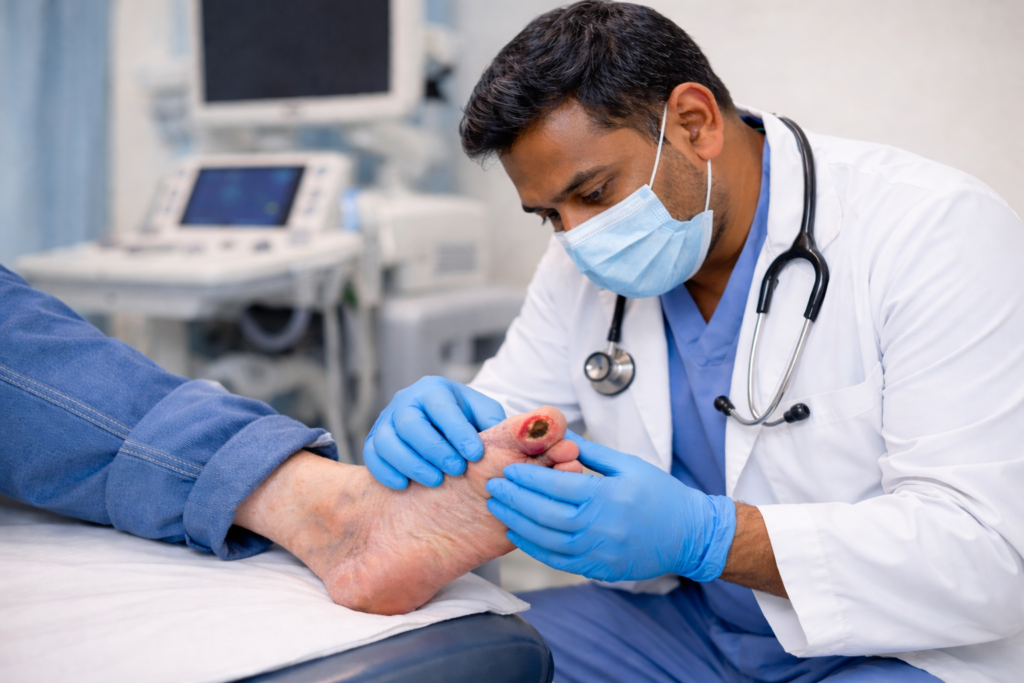
Many diabetic patients suffer from neuropathy (nerve damage), meaning they can’t feel a pebble in their shoe or a developing blister. Because you can’t feel the pain, a small nick can quickly turn into a deep ulcer.
A vascular surgeon doesn’t just treat the wound; we evaluate the entire circulatory system. We use specialized tests to measure exactly how much oxygen is reaching your toes. By catching poor circulation early—even before a wound appears—we can prevent the tissue death that leads to amputation.
The Goal: Limb Preservation
The ultimate goal of a vascular surgeon is Limb Salvage. We look at the “big picture” of your health:
- Restoring Flow: Ensuring the foot has enough blood to heal.
- Infection Control: Working with other doctors to stop the spread of bacteria.
- Healing: Providing the vascular foundation that allows wound care treatments to actually work.
When to See Us
You should ask for a vascular evaluation if you have diabetes and notice:
- A sore or ulcer that hasn’t improved in two weeks.
- Your feet feel cold to the touch or look pale/blue.
- Pain in your calves while walking that goes away with rest.
- Rest pain (pain in your feet that keeps you up at night).
Remember: In the world of diabetic foot care, “Time is Tissue.” Addressing circulation issues early is the most effective way to stay mobile and keep your feet healthy.
